Abstract
Background: Benign non-functioning pituitary macroadenomas (NFMA) often cause mass effect on the optic chiasm necessitating transsphenoidal surgery to prevent blindness. However, surgery is complicated and there is a high tumour recurrence rate. Currently, very little is known about the natural (and residual post-surgical) growth patterns of these NFMA. Conflicting data describe decreased growth to exponential growth over various time periods. Due to lack of information on growth dynamics of these NFMA, suitable follow-up imaging protocols have not been described to date.
Objective: To determine if NFMA grow or stay quiescent over a time period using serial MRI investigations and a stereological method to determine tumour volume. In addition, to evaluate if NFMA adhere to a certain growth pattern or grow at random.
Method: Thirteen patients with NFMA had serial MRI investigations over a 73-month period at the Universitas Academic Hospital. Six of the selected patients had undergone previous surgery, while seven patients had received no medical or surgical intervention. By using a stereological method, tumour volumes were calculated and plotted over time to demonstrate growth curves. The data were then fitted to tumour growth models already described in literature in order to obtain the best fit by calculating the r2 value.
Results: Positive tumour growth was demonstrated in all cases. Tumour growth patterns of nine patients best fitted the exponential growth curve while the growth patterns of three patients best fitted the logistic growth curve. The remaining patient demonstrated a linear growth pattern.
Conclusion: A specific growth model best described tumour growth observed in non-surgical and surgical cases. If follow-up imaging confirms positive growth, future growth can be predicted by extrapolation. This information can then be used to determine the relevant follow-up-imaging interval in each individual patient.
Introduction
Pituitary adenomas are almost always benign (>99.9%), arise from the anterior pituitary and account for approximately 15% of all intra-cranial tumours.1,2 The majority of these adenomas show no local invasion of bone, cavernous sinus or vascular encasement and malignant transformation and metastases are extremely rare (0.2% of all adenoma cases).2,3
Pituitary adenomas can be divided into microadenomas (< 1 cm) or macroadenomas (> 1 cm) according to their widest diameter.1,4 The prevalence of pituitary adenomas in the general population has been reported to be 10%–27%, with macroadenomas considerably lower at 0.2%.5 Macroadenomas are predominantly non-functioning (> 80%),5,6 that is, there is no clinical and biochemical evidence of pituitary hormonal overproduction and serum prolactin levels of ≤ 100 ng/mL are required for classification as such.1,5
Non-functioning pituitary macroadenomas (NFMA) are the most prevalent pituitary neoplasm and their growth is haphazard with lobulation.7 Growth normally occurs through the diaphragma sellae into the suprasellar cistern with a characteristic ‘snowman’ appearance.1
Clinically, patients present with visual field defects, headache or hypopituitarism due to NFMA mass effect on surrounding structures.2,4,5 It is well accepted that once visual disturbances are present, transsphenoidal surgery is required to prevent blindness.6,8 Although up to 80% of patients experience significant visual improvement post-surgery,6,8 it is a technically difficult procedure with a high tumour recurrence rate of 12%–46%.4,5 Multi-lobulated macroadenomas with vertical suprasellar expansion are less likely to be totally removed than round tumours.9 Apoplexy is another possible complication seen in approximately 5% of cases.10 It is defined as infarct or haemorrhage in the pituitary gland, most likely due to alterations in perfusion pressure.2,10
Incidentally detected pituitary adenomas represent 20%–
40% of all NFMA.3,7 Asymptomatic non-functioning macroadenomas incidentally found on imaging pose a treatment dilemma. In the absence of visual symptoms, the neurosurgeon may opt for an expectant approach although complications like apoplexy, blindness and hypopituitarism may occur.5 In addition, the time interval between imaging and performing surgery on these patients remains unclear.8
A meta-analysis by Ezzat et al. found that the prevalence of pituitary adenomas is 14.4% in autopsy studies and 22.5% in radiological studies.11
Due to uncertainty regarding growth of pituitary adenomas, various authors have attempted to study their growth over a selected time period. In a series of pituitary adenomas detected incidentally, Donovan and Corenblum,7 found positive growth in 4 of 16 large tumours (> 1 cm in height) but no growth in 15 tumours smaller than 1 cm in height over 6.1 and 6.7 years, respectively. This suggests that a small percentage show considerable growth but the majority remain stable. Tumour enlargement thus seems more predominant in macroadenomas compared with microadenomas.11 Reincke et al.12 also noted an increase in tumour height in three of 14 incidentalomas monitored over 22 months. Average tumour height was 13 mm with a range of 5 to 25 mm in diameter.
Dekkers et al.8 investigated the natural growth course of NFMA. Growth was defined as a 0.01 cm increase in size in any direction and positive growth was shown in 14 of the 28 cases. They used an ellipsoid formula to approximate tumour volume but unfortunately this method does not allow for the measurement of irregular edges. In addition, a spontaneous decrease in tumour volume was reported in 29% of patients.
Growth of postoperative residual adenomas has also been studied. Turner et al.13 observed tumour regrowth in 21 of 65 patients over a 76-month follow-up period.
However, in all of the mentioned studies; however, heterogeneous criteria were used for defining tumour growth. Tumour height was seen as the most important predictor of optic chiasm compression resulting in calculations based on tumour height only.3 Other authors calculated initial and end tumour volumes with no description of the actual growth pattern. Thus, these studies failed to provide suitable quantitative information on the actual growth velocity of pituitary macroadenomas.
Tanaka et al.14 used the first volumetric assessment technique to calculate tumour volume by scanning the tumour outline on a computer. Regrowth was seen in 38 of 40 residual post-surgical tumours mostly in an exponential fashion.
Honneger et al.11 performed the first quantitative assessment of growth on incidentalomas in post-surgical cases. They used the stereological method to calculate tumour volume based on calculating tumour area on each contiguous slice. They found statistically significant exponential tumour growth in the majority of cases which enabled them to suggest a follow-up imaging protocol for patients.
Based on the results from studies done to date, the stereological method is the most accurate way to assess tumour volumes on imaging because it accommodates the haphazard growth often observed.
In this study, the NFMA growth pattern and rate was determined in a South African population using the stereological method used by Honneger et al.11 Measurements were, however, taken in two planes from thin MRI slices to increase measurement accuracy. The growth patterns observed were then fitted to mathematical growth models described in literature.
Research method and design
Approval was obtained from the University of the Free State Ethics Committee as well as the National Health Research Database in the Free State prior to study commencement.
Retrospective data were collected from patients who received follow-up MRIs between 29 October 2008 and 10 November 2014 at the Universitas Academic Hospital in Bloemfontein. Suitable cases were chosen from the information available from 46 patients on the database. Informed consent was therefore not required for this study. Subjects were assigned random numbers and are referred to as such.
Patient selection was based on benign macroadenoma appearance on imaging regardless of age, race or sex. Histological confirmation of pituitary macroadenoma was required in post-surgical cases. NFMA also had to be classified as non-functional in order to ensure that dopamine antagonists were not concomitantly used, which might have caused a decrease in tumour size. Potential patients were therefore required to have a baseline serum prolactin level of below 100 ng/mL and these results were obtained from the University National Health Laboratory Service (NHLS).
Serial MRI investigations of 13 patients (3 women and 10 men) from the age of 25 years to 69 years who had all the necessary evaluations done according to the above criteria, were studied over a 73-month period. Vertical tumour measurement had to be more than 1 cm and all patients had received between three and six serial MRI investigations.
Six of these patients had undergone initial adenoma surgery, and only follow-up imaging was used for calculations. Post-surgery imaging was typically done within 3 months after the initial procedure. The remaining seven patients had received no medical or surgical intervention. The decision to withhold surgery was made by the managing clinicians and reasons included patients declining surgery, carotid artery encasement and poor anaesthetic risk. Patients with apoplexy were excluded as this could have influenced tumour volume.
The average tumour volume was calculated from the measurements in two planes (sagittal and coronal). The primary researcher did the measurements on two separate occasions under the direct supervision of a neuroradiologist. The average of these two values was then used to calculate the in-depth volumetric assessment according to the stereological model.
Materials
All MRI investigations were obtained with a 1.5 tesla MRI machine (General Electric, Signa Dual Gradient, Milwaukee, USA).
Procedure
- Thin MRI slices in the coronal and sagittal planes were studied in all cases. All patients received intravenous gadolinium at a dose of 0.2 mL/kg.
- A standard imaging protocol was used for all patients:
- Field of view = 20 mm2
- Matrix = Frequency 320 × Phase 224
- Slice thickness between 2 and 5.0 mm
- Spacing between 0.2 and 0.5 mm
- Number of excitations = 5.
A stereological method was used to obtain tumour volumes in both sagittal and coronal planes. Tumour edges were outlined by free-hand on each slice and then the respective two-dimensional area was calculated using an imaging processing software program (Isite) available on the Patient Archive and Communication System (PACS). Tumour volume was calculated on standard radiology reporting monitors.
Tumour area (measured in cm2) on each slice was then multiplied by the sum of the slice thickness and the intervening gap to calculate the volume of one slice. All values were then added to estimate the total tumour volume for each serial MRI investigation. All tumour volumes were measured in cm3 and all time periods were recorded in days.
The data were captured into Microsoft Excel before submission to the Department of Biostatistics for further statistical analysis.
Analyses
Average tumour volume of the sagittal and coronal planes was plotted using at least four consecutive data points and fitted to the following three established mathematical models:
- Logistic: Initially exponential growth followed by a linear growth phase and finally approaching a constant plateau.
- Exponential: During a period of time there is a constant percentage increase in tumour volume.
- Linear: Constant increase in tumour volume.
- The ‘goodness of fit’ was obtained by calculating the square of the correlation coefficient (r2 value). For patients with insufficient data points, the r2 value could not be calculated. Growth was nonetheless described based on the shape of the observed curve when plotted using the available points.
Results
Figure 1 demonstrates six serial T1 weighted post-contrasted MRI slices through the tumour in the coronal plane. As demonstrated in Figure 2a and Figure 2b, these tumours often have lobulated outer margins.
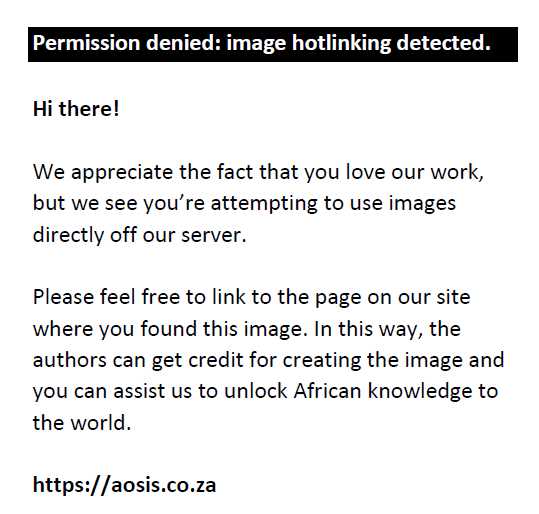 |
FIGURE 1: Non-functioning pituitary macroadenoma in a 46-year-old male. |
|
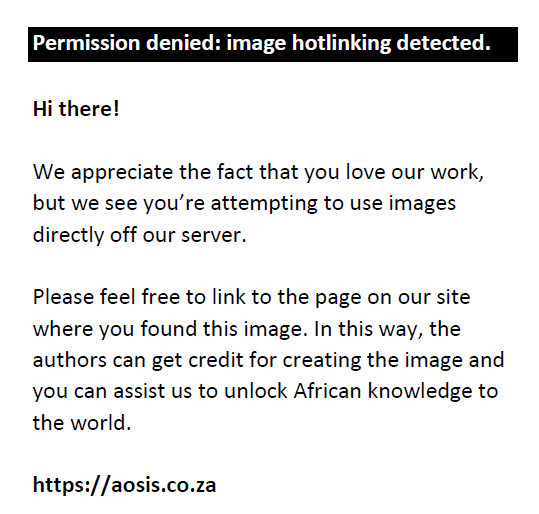 |
FIGURE 2: Large non-functioning pituitary macroadenoma in a 54-year-old male: Sagittal (a) and coronal (b) T1-weighted images (post-contrast) of the brain. |
|
All subjects demonstrated positive tumour growth over the observation period (Table 1). The initial measured median tumour volume was 11.96 cm3 compared to an end median volume of 19.00 cm3 after the 73-month period.
| TABLE 1: Clinical data, imaging studies as well as growth patterns observed during the observation period. |
In nine cases, NFMA growth was best demonstrated by an exponential curve. Of these, three had sufficient data points to calculate the r2 value. Higher r2 values for the exponential model (mean r2 = 0.99) were found compared with the logistic model (mean r2 = 0.95). No statistical significance was found when comparing the exponential to the logistic growth patterns (p = 0.06). Observed growth that best fitted the exponential model had an r2 value of 0.97 (Figure 3). Of the nine cases, three had received surgery and six had been treated conservatively. The initial mean volume was 16.24 cm3 (±10.15) and end volume was 25.69 cm3 (±16.03). The minimum initial tumour volume was 2.68 cm3 and maximum tumour end volume was 52.08 cm3.
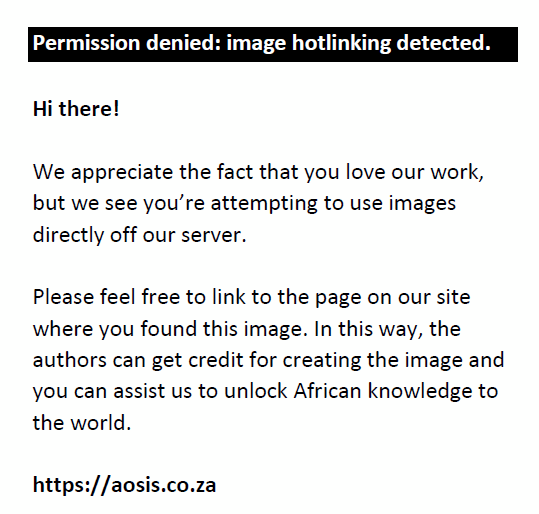 |
FIGURE 3: Macroadenoma growth observed in a 46-year-old male. |
|
The logistic model best described three cases, with only two patients having sufficient data points to calculate the r2 value. Of these, a mean r2 value of 0.94 was seen compared with a mean r2 value of 0.85 in the exponential model. No statistical significance was found on comparing the logistic and exponential growth patterns (p = 0.37). Observed growth that best fitted the logistic growth model had an r2 value of 0.94 (Figure 4). In two of the cases, the patients had received surgery and, in one case, the patient had received conservative treatment only. The initial mean volume was 2.33 cm3 (±2.77) and end volume was 2.92 cm3 (±3.64). The minimum initial volume was 0.70 cm3 and maximum end volume was 7.13 cm3.
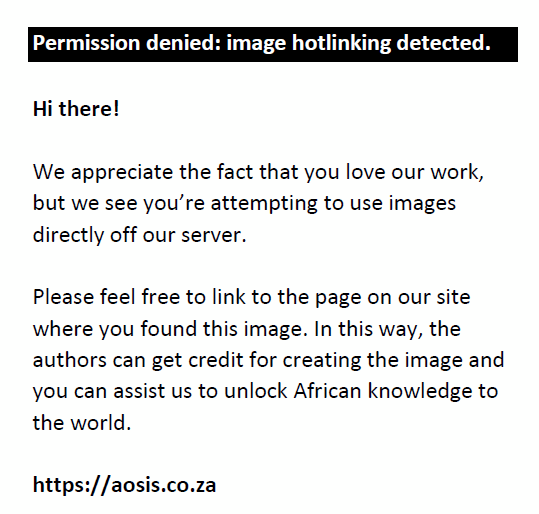 |
FIGURE 4: Macroadenoma growth observed in a 25-year-old female. |
|
Only one case exhibited a linear trend; however, there were insufficient data points to calculate the r2 value. This patient had received surgical intervention. Initial tumour volume was 2.35 cm3, and end volume was 7.01 cm3.
In adherence to exponential growth, the five largest tumours, with an initial calculated volumes of more than 15 cm3 demonstrated a higher average growth rate of 5.15 cm3/year compared with 1.10 cm3/year seen in tumours smaller than 15 cm3. Furthermore, tumours adhering to the exponential growth pattern had an average initial size of 16.24 cm3 compared with 2.33 cm3 seen in the logistic pattern.
Discussion
Mathematical modelling has been applied to describe growth of other tumours in literature. Experimental tumour paradigms of malignant and rapidly growing tumours typically adhere to a sigmoidal curve (Figure 5). This is described as the logistic mathematical model: an exponential phase followed by a linear phase and lastly, a plateau phase. Final deceleration is likely due to impaired blood supply with central necrosis and restricted growth in the peripheral regions.11
 |
FIGURE 5: Logistic growth curve representing growth observed in malignant tumours. |
|
However, in contrast to malignant tumours, NFMA are benign, homogenous and solid, and it is hypothesised that they should show stable growth behaviour. If the entire volume of a solid tumour grows at a constant rate, exponential tumour growth would be expected resulting in a constant tumour volume doubling time.11
All the patients in this study showed an increase in tumour volume over time. It seems that when volumetric assessment is applied on high quality imaging, the incidence of growth is much higher compared with previous studies. On follow-up imaging, the tumours often appeared unchanged in size only to find a significant volume increase after the necessary calculations. This contrasts the spontaneous decrease in tumour volume reported in 29% of patients in the study by Dekker et al.11 A decrease in volume is, however, highly improbable due to the solid nature of these tumours.
No clear trend in the tumour growth patterns could be deducted for conservatively treated adenomas versus post-surgical cases or in different age groups.
Observations of this study were similar to those of Honegger et al.,11 with the majority of cases (69%) adhering to the exponential growth model. In the five cases with enough data points, high r2 values for the exponential and logistic models were obtained, but the p-value was not statistically significant to classify growth into a specific model. In cases with insufficient data points, the graph trend was used to classify growth to a specific growth model.
Larger initial mean NFMA (16.24 cm3) tend to show exponential growth when compared with smaller tumours (2.33 cm3), which exhibited logistic growth. On an individual case level, however, initial tumour size cannot be used to accurately determine the growth velocity or pattern (e.g. patient 1 who demonstrated exponential NFMA growth had an initial tumour volume of 2.68 cm3, and patient 2 who showed logistic NFMA growth had an initial volume of 5.54 cm3).
The hypothesis that adenomas with an exponential pattern would eventually follow a logistic growth pattern could not be determined due to the fixed observation period.
One patient demonstrated adherence to the linear model; however, it can be postulated that the NFMA might have been in the linear growth phase of the logistic model.
These results demonstrate that if there is a significant increase in growth at first follow-up, exponential or logistic growth can be expected in future. If no increase in growth is found, it is unlikely that the tumour will grow rapidly in the near future. Once the individual patient trends are established, appropriate and effective treatment can be prescribed for these patients, which includes a follow-up MRI-protocol tailored for each individual.
Limitations of the study
The lack of long-term follow-up due to the fixed observation period was seen as a study limitation. As a result, the possibility that these benign tumours would eventually demonstrate logistic growth could not be determined.
Conclusion
Based on these results, it can be recommended that radiologists calculate tumour volume using this stereological method on serial MRI imaging to determine the growth rate. In conjunction with imaging, regular follow-up regarding ophthalmology evaluation and hormonal assessment is advised.
This insight into the growth dynamics of NFMA may facilitate the development of a tailored follow-up imaging protocol for patients with either incidentalomas or post-surgical NFMA. This may reduce healthcare expenses by allowing an individualised rational treatment plan.
Acknowledgements
The first author would like to thank Dr Otto for reviewing the measurement process, Prof. De Vries for his guidance as study leader, the Department of Neurosurgery for providing the subject information, the National Health Laboratory Services for assisting me with the relevant blood results and the Department of Biostatistics at the UOFS.
Competing interests
The authors declare that they have no financial or personal relationships which may have inappropriately influenced them in writing this article.
Authors’ contributions
C.S.d.V. was the project leader. J.P. performed the measurements and performed all the calculations and S.F.O. made conceptual contributions and supervised the measurement process.
References
- Dekkers OM. Nonfunctioning pituitary macroadenomas: Treatment and long-term follow-up. PhD Thesis. Universiteit Leiden; 2006.
- Mamelak AN, Carmichael JD, Park P, Bannykh S, Fan X, Bonert HV. Atypical pituitary adenoma with malignant features. Pituitary 2011;14(1):92–97. http://dx.doi.org/10.1007/s11102-008-0151-1
- Berkmann S, Schlaffer S, Buchfelder M. Tumor shrinkage after transsphenoidal surgery for nonfunctioning pituitary adenoma. J Neurosurg 2013;119(6):1447–1452. http://dx.doi.org/10.3171/2013.8.JNS13790
- Arita K, Tominaga A, Sugiyama K, et al. Natural course of incidentally found nonfunctioning pituitary adenoma, with special reference to pituitary apoplexy during follow-up examination. J Neurosurg. 2006;104(6):884–891. http://dx.doi.org/10.3171/jns.2006.104.6.884
- Dekkers OM, Pereira AM, Romijn JA. Treatment and follow-up of clinically nonfunctioning pituitary macroadenomas. J Clin Endocrinol Metab. 2008;93(10):3717–3726. http://dx.doi.org/10.1210/jc.2008-0643
- Turner HE, Stratton IM, Byrne JV, Adams CB, Wass JA. Audit of selected patients with nonfunctioning pituitary adenomas treated without irradiation – A follow-up study. Clin Endocrinol (Oxf) 1999;51(3):281–284. http://dx.doi.org/10.1046/j.1365-2265.1999.00865.x
- Honegger J, Ernemann U, Psaras T, Will B. Objective criteria for successful transsphenoidal removal of suprasellar nonfunctioning pituitary adenomas. A prospective study. Acta Neurochir (Wien). 2007;149(1):21–29. http://dx.doi.org/10.1007/s00701-006-1044-6
- Dekkers OM, Hammer S, de Keizer RJW, et al. The natural course of non-functioning pituitary macroadenomas. Eur J Endocrinol. 2007;156(2):217–224. http://dx.doi.org/10.1530/eje.1.02334
- Donovan LE, Corenblum B. The natural history of the pituitary incidentaloma. Arch Intern Med. 1995;155(2):181–183. http://dx.doi.org/10.1001/archinte.1995.00430020067008
- Lee J-S, Park Y-S, Kwon J-T, Nam T-K, Lee T-J, Kim J-K. Radiological apoplexy and its correlation with acute clinical presentation, angiogenesis and tumor microvascular density in pituitary adenomas. J Korean Neurosurg Soc. 2011;50(4):281–287. http://dx.doi.org/10.3340/jkns.2011.50.4.281
- Honegger J, Zimmermann S, Psaras T, et al. Growth modelling of non-functioning pituitary adenomas in patients referred for surgery. Eur J Endocrinol. 2008;158(3):287–294. http://dx.doi.org/10.1530/EJE-07-0502
- Glass RM, Drummond W, Cole HΜ, et al. The ‘incidentaloma’ of the pituitary gland. Is neurosurgery required? J Am Med Assoc. 1990;263(20):2772–2776. http://dx.doi.org/10.1001/jama.1990.03440200076026
- Anagnostis P, Adamidou F, Polyzos SA, Efstathiadou Z, Panagiotou A, Kita M. Non-functioning pituitary adenomas: A single center experience. Exp Clin Endocrinol Diabetes. 2011;119(5):314–319. http://dx.doi.org/10.1055/s-0030-1267991
- Tanaka Y, Hongo K, Tada T, Sakai K, Kakizawa Y, Kobayashi S. Growth pattern and rate in residual nonfunctioning pituitary adenomas: Correlations among tumor volume doubling time, patient age, and MIB-1 index. J Neurosurg. 2003;98(2):359–365. http://dx.doi.org/10.3171/jns.2003.98.2.0359
|